Building community: supporting eating disorder awareness in schools

Eating Disorders Awareness Week 2026 highlighted the power of community, with schools playing a crucial role in supporting young people at risk. In response to rising clinical complexity and the need for earlier intervention, our team delivered targeted training to educational settings – strengthening collaboration, improving recognition and enhancing support for students with eating disorders.
The theme of BEAT’s Eating Disorders Awareness Week this year was community.[1] When my team and I began thinking about this, we unanimously felt that schools are a vital part of our wider community that support the young people who access our service.
An emerging theme we identified was that new referrals coming into the service were showing an increase in the level of physical health risk. This often leads to an increase in hospital admissions at the beginning of treatment, which can be disruptive and traumatic for the families and young people undergoing treatment. At times this impacts therapeutic relationships with the team and engagement with longer term therapeutic support. In some cases, this leads to prolonged support required under the community team.
Offering training in educational settings felt in keeping with the newly published National Guidance for Eating Disorder Services for Children and Young People, which highlights the importance of collaborative working between community eating disorder services and educational settings.[2] The guidance outlines the importance of early intervention from community eating disorder services and supporting educational settings regarding recognition and awareness of eating disorders. Therefore, targeting schools felt like the perfect place to focus our efforts.
Response from schools
Initially when reaching out to schools I was unsure of what the response would be, given how busy teaching and pastoral staff are. We had an overwhelmingly positive response; 13 out of 15 schools quickly replied, jumping at the chance for support in this area. On average, we had 10–25 attendees from each school.
Our offering
Our aim when setting out the training was to improve overall awareness of the types of eating disorders, and the impact they can have on physical and mental health. We also aimed to increase knowledge about how to recognise signs of eating disorders, initiate discussions with young people when there are early signs of concerns and discuss how to complete timely referrals.
In the presentation, we shared an overview of our service, details of types of eating disorders the service is/is not commissioned to treat, causes of eating disorders, people more predisposed to developing an eating disorder and the higher prevalence in those with a diagnosis of autism and/or ADHD. Physical health signs and symptoms to be aware of and when to be concerned were also covered.
We felt it was important to share the clinical guidance we follow to monitor/manage this risk. The Managing Emergencies in Eating Disorders (MEED) tool was shared and discussed.[3] This allowed us to provide context as to why we may be advising young people to be on a reduced timetable or have time off school to focus on eating disorder treatment at home and conserve energy – particularly if their level of physical health risk was in the red or amber section of MEED, which indicates risk to life.
Finally, we covered how school could support treatment. The input from schools varies across the area. In some cases, teaching and pastoral staff are very involved and able to support with mealtime supervision. In other cases, schools have more of a support role but remain vital in picking up on students who may be struggling and need early referral.
The secretive nature of eating disorders can leave parents unaware or ambivalent to their children’s struggles. As a team we have noticed cases where teachers have been able to recognise patterns in behaviour, such as social isolation and becoming more withdrawn, or visible differences in weight loss and overall appearance (particularly following return from summer holidays).
Feedback from schools
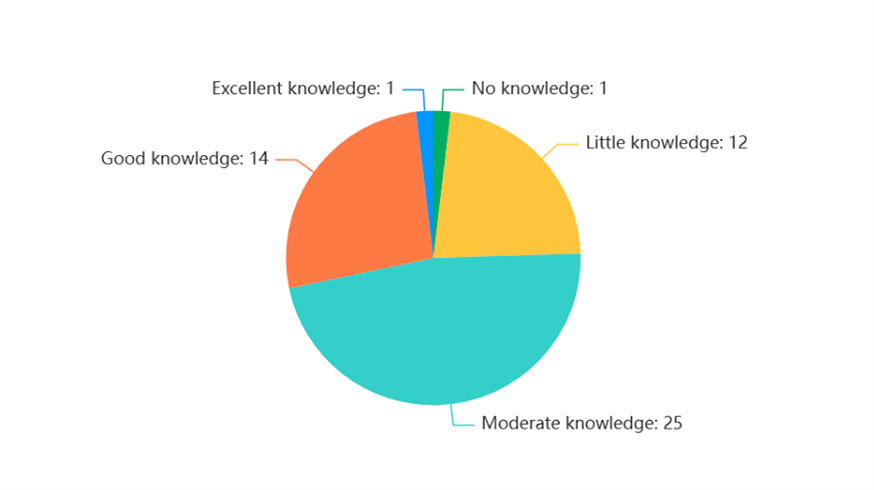
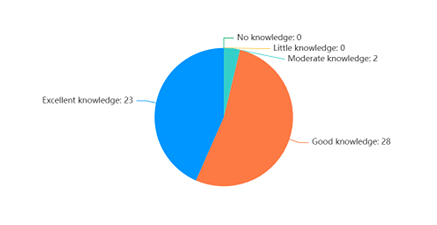
Survey data collected from the training supports indicates that we achieved our training goals. Figure 1 shows the varied levels of knowledge relating to eating disorders prior to the training. Figure 2 shows that knowledge improved overall post-training delivery.
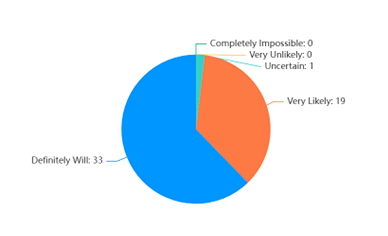
We were pleased to see that the feedback shows the level of confidence in completing a referral to the eating disorder team after training was high, as shown in Figure 3.
Emerging topics that came from the feedback and questions during the training demonstrated that educational settings were noticing the impact of social media, in particular, trends for eating habits and body standards. Another topic across all schools was the impact of busy environments at break times in canteens affecting dietary intake, alongside the general culture of students not eating lunch in schools (or drinking) due to not wanting to use the toilets.
Many schools highlighted the increase in trends surrounding young males in terms of excessive exercise, clean eating and high protein intake. Some teachers raised concerns about the possible use of substances to build muscle in the quest to achieve a desired physique.
Further support, such as education sessions direct to students, was requested by many schools. As a team we reflected that this would need careful consideration around achieving the balance of increasing knowledge and awareness, without discussing topics with those more vulnerable and potentially triggering any negative thoughts/behaviours.
Conclusion
As a team, we thoroughly enjoyed celebrating the theme of community for Eating Disorder Awareness Week and acknowledging how important all wider teams/professionals are to our day-to-day work and to the young people we support. The key points we gained from the training are:
The benefit of offering face-to-face training to improve professional relationships and strengthen future joint working. Being able to put a face to a name behind an email or online video call feels beneficial.
Being able to view the school sites ourselves; this insight will be vital when considering reduced timetables or time off school due to the impact school can have in terms of energy expenditure. The size of school sites was vastly larger than we had anticipated.
The appreciation for our team taking the time to share our knowledge and support was lovely to see.
We work in a niche area of mental health, but one that can have a huge impact on young people and the lives of their families. It feels important to share our team’s experience and expertise.

Sarah Dukes RD is a Specialist Eating Disorder Dietitian and Clinical Co-ordinator at Cheshire and Wirral Partnership NHS Trust. She is currently working as a specialist eating disorder dietitian and clinical co-ordinator in CAMHS eating disorder team.
Sarah Dukes RD
References:
Beat. The UK’s eating disorder charity. The UK's Eating Disorder Charity - Beat. Accessed March 23, 2026
NHS England. Eating disorder services for children and young people: National Guidance. Published January 20, 2026. Accessed March 23, 2026 https://www.england.nhs.uk/publication/eating-disorder-services-for-children-and-young-people-national-guidance
Royal College of Psychiatrists. Medical emergencies in eating disorders: guidance on recognition and management (MEED). Royal College of Psychiatrists; 2022. Accessed March 23, 2026 https://www.rcpsych.ac.uk/docs/default-source/improving-care/better-mh-policy/college-reports/college-report-cr233-medical-emergencies-in-eating-disorders-(meed)-guidance.pdf

Comments