Paediatric News and Research
Essential resources and information hub for paediatric dietitians, nutritionists and healthcare professionals with an interest in paediatrics.
Caregiver response is key to emotional overeating in children
July 2024
A recent study from the University of Illinois following children from birth to age three, has revealed a strong link between caregiver responses to children's negative emotions and the development of emotional overeating. Whilst a child's temperament plays a role, how parents or caregivers handle their child's distress, fear, or anger significantly impacts whether the child turns to food for emotional comfort. Supportive responses, such as problem-solving or validating feelings, can help prevent emotional overeating, while punitive or dismissive reactions increase the risk.
Co-author of the study, Samantha Iwinski said that their findings highlight the "importance of the family system."
"Behaviours at three months of age can affect children when they are three years old... assistance may be needed at multiple developmental milestones," said Iwinski.

Characterising glycosaminoglycans in human breast milk and their potential role in infant health: new review

July 2024
A recent review published in Microbial Cell looked at the literature on glycosaminoglycans in human breast milk and their potential role in infant health.(1)
The review focused on glycosaminoglycans (GAG), identifying the challenges of research in this area due to the complexities of extraction and analysis.
It is commonly known that the composition of breast milk changes from the early-stage colostrum to transitional milk and mature milk. The bioactive components are reduced and the nutritional components increase. Composition can also be affected by maternal obesity, stressful birth, poorly managed diabetes and maternal diet and stores, to name a few.
The review highlights the importance of GAG in immune function and gut function. However, it notes that the research on the mechanisms needs to be more robust. Aliya Porter, RNutr
1.Greenwood, M. et al (2024). Characterising glycosaminoglycans in human breastmilk and their potential role in infant health. Microbial Cell 11: 221-234. doi: 10.15698/mic2024.07.827. https://microbialcell.com/researcharticles/2024a-greenwood-microbial-cell/
New review on MDT experiences and perceptions of blended diet
June 2024
We know from the Hub article this month that the use of blended diet is becoming more common. In a new review, Clancy et al (2024) looked at the experiences and perceptions of the multidisciplinary team (MDT) regarding blended diet in children in Ireland, The study was conducted across three sites in Ireland and included doctors, nurses and eligible AHPs (dietitians, speech and language therapists, physiotherapists, occupational therapists, psychologists and medical social workers).
The response rate was 80.3% with a 32.9% response from doctors, 31.9% from nursing staff and 15.5% from dietitians. 33.9% reported they had not heard of blended diet and of those who had heard of it, 68.1% had delivered care to a child/young person on blended diet. 70% of responders felt able to recommend blended diet to a family as a feeding option. 42.9% of responders who had experience of blended diet felt unable to recommend it as a treatment option, as they felt they were not competent in this area.
A key reason to recommend blended diet was parental desire (39.5%) and dietitians reported that current symptoms accounted for 55% on recommendations to consider starting blended diet. Almost 42% reported family logistics as a barrier to commencing blended diet, whilst 20.9% were concerned regarding nutritional adequacy of blends. 92.4% of responders expressed an interest in receiving further information on blended diets, including information on the evidence base (24.7%), how to monitor the diet (25.6%) and how to plan a nutritionally balanced blended diet (22.6%).
This is the first study exploring MDT perceptions of blended diet in Europe and provides useful information for the needs of healthcare professionals to enable the provision of blended diet to move forward. Clancy et al (2024) conclude that healthcare settings should provide evidence based training to healthcare professionals on blended diet, which would optimise the treatment and safety of young people in their care. Hazel Duncan, RD
Nutrition management in children with severe neurological impairment: latest narrative review
June 2024
The nutritional management of children with severe neurological impairment can be highly complex and, as life expectancy increases, the nutritional management of these young people can become more challenging. Oftedal et al (2024) have carried out a narrative review looking at the progression of the nutritional management of this patient group.
Over the decade there has been marked development in the assessment of this patient group’s nutritional status, with development of tools to help assess ability. The challenges are clear around measuring length and body composition and often repeated accurate measurements of skinfold thicknesses or bioelectrical impedance can be useful to determine body composition alongside weight. However, these alternative measurements can be difficult to assess accurately and ensure consistency if various staff are involved. As dietitians, we recognise that children within this patient group will grow differently to their peers and that poor growth does not directly correlate to poor nutrition.
Gastrointestinal symptoms are commonly reported to be problematic, with a large number of these patients receiving tube feeding to ensure nutritional requirements are met. Whilst there is increased evidence base around the positive impact of fibre on the gut microbiome, there is limited evidence around the use of fibre in this specific patient group. Nevertheless, from the information available, the addition of fibre is positive for children and young people.
GI DYSTONIA: EMERGING EVIDENCE
Gastrointestinal dystonia is a ‘new diagnosis’, which has been defined to capture the challenges that we see when feeding these complex children and young people. GI dystonia is a term used to encompass symptoms of distress (pain behaviour, hypertonicity, retching, vomiting, vagal phenomenon and abdominal distension). The best treatment for GI dystonia is not fully understood, but emerging evidence would suggest that tube feeding using blended diet may be beneficial. Even without the presence of GI dystonia there has been an increased use in blended diets within this patient group, which has reported benefits in the management of gastrointestinal symptoms. The development of new interventions to support eating and development skills is being viewed as a positive step towards supporting these families.
The nutritional management of children and young people with severe neurological impairment is challenging for dietitians and healthcare professionals. An experienced dietitian is key in assessing and interpreting growth and providing strategies to improve long-term health outcomes. The authors conclude there is a balance to be found between adequate nutrition to support growth, development and well-being without over feeding and the detrimental impact this would have on these young people. Hazel Duncan, RD

May 2024
A report from the Access to Nutrition Initiative published in January 2024 compared over 1000 products marketed to infants and young children with the WHO Nutrient and Promotion Profiling Model (NPPM) developed in 2022. Most companies (81%) met NPPM requirements for fat, fruit content, sodium, and protein (>81%), however, only approximately 35% of all assessed products met all nutrient composition criteria and none of the companies met all of the labelling requirements. It highlights the need for further work in this area. The full report can be found here. Aliya Porter, RNutr

May 2024
First Steps Nutrition Trust has released a new guide: Eating Well: 6 months to 2 years for South Asian Children. This was first written as part of the NEON study (https://www.acesoghc.com/neon) in 2021 but has now been released for general use. It can be found here...
The guide can be used with families to support healthy eating messages and good practice around responsive feeding. It is free to download. Aliya Porter, RNutr
The evolving role of dietitians in neonatal units - report findings
18th April 2024
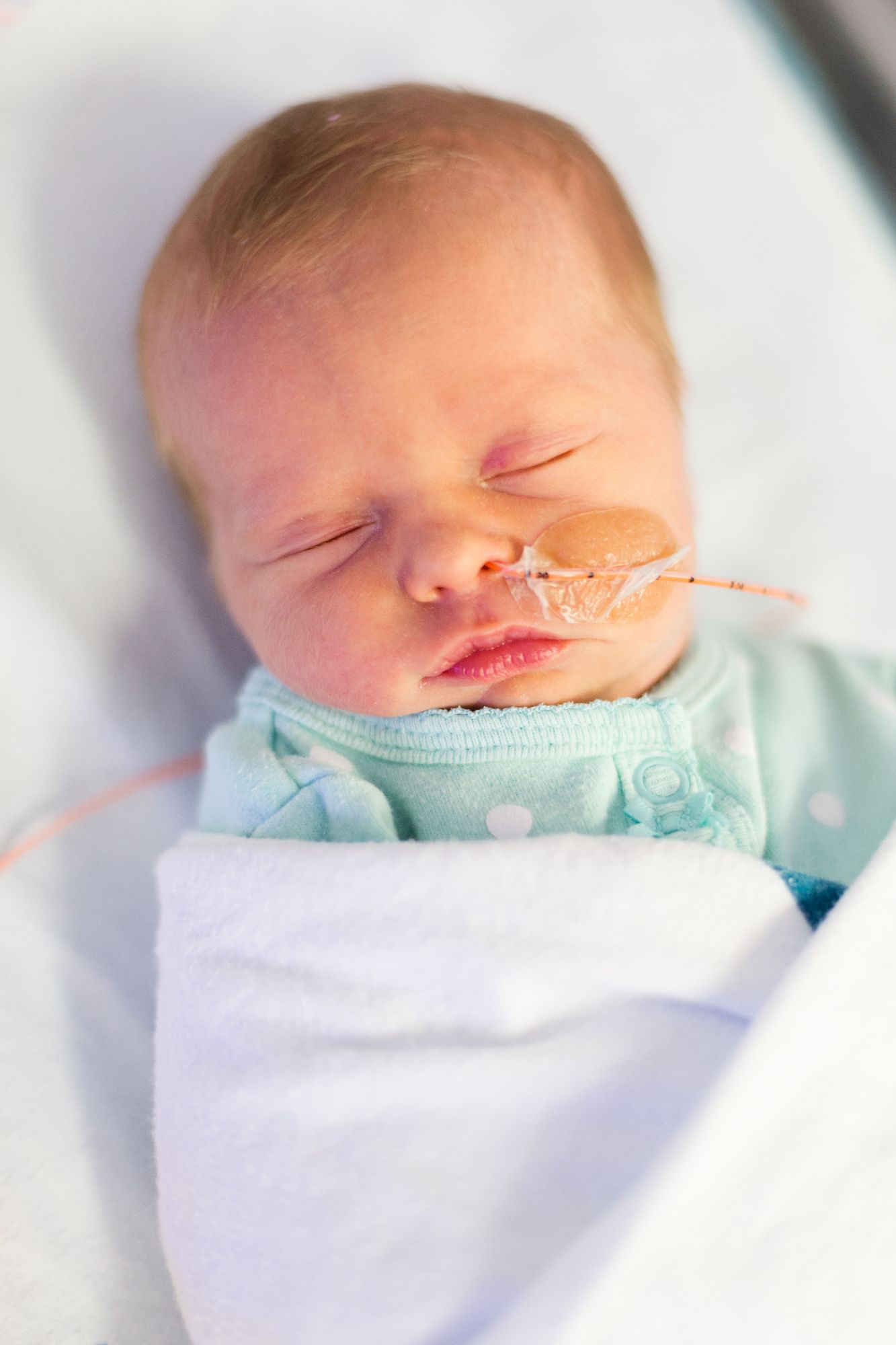
The number of infants born prematurely is increasing and neonatal medicine has advanced dramatically over the last 30 years, with infants born around 21-22 weeks gestation now being given a 0-10% chance of survival. As neonatal care is developing and the infants are having better outcomes, the focus of care is shifting to ensure infants are thriving with the best opportunities. Nutritional care from an experienced neonatal dietitian is recognised in being fundamental in optimising outcomes for these complex young patients. Smith & Mustapha (2024) have presented an article highlighting the evolving role of dietitians in neonatal units and beyond and offer recommendations for the scope of work required.
Dietitians should be embedded within the neonatal unit and as part of the wider multidisciplinary team. They should be able to provide individual assessments and adapt care plans for complex patients when they fall out with standard guidelines. Neonatal dietitians should be involved in the development of care pathways for specific groups such as the provision of parenteral nutrition and the use of breast milk fortifier. Neonatal dietitians should be present and involved in nutrition and developmental care ward rounds and should be involved in universal care improving awareness of nutrition-related topics for staff and parents.
Neonatal dietitians are recognised to improve nutritional outcomes for their patients by providing evidence-based holistic care at a time-critical neonatal period. This improves both recovery and long-term health outcomes. Improved nutritional status is in turn linked to increased survival rates, attenuation of the effects of critical illness and improved neurodevelopmental outcomes. Dietetic provision within this patient group can lead to reduced length of hospital stay.
Smith & Mustapha (2024) go on to recognise that neonatal dietitians have an ongoing responsibility to provide timely and effective follow-up to these patients and families to bridge the gap between hospital and home. Neonatal dietitians can also provide practical, realistic advice around weaning the premature infant and should also be part of the MDT assessing infants at neuro-developmental follow-up clinics.
The review presented by Smith & Mustapha has highlighted the essential role and key benefits of experienced neonatal dietitians at unit, community and network level. Neonatal dietitians can have a vast and diverse impact on the care of infants in the appropriate units and provide holistic and expert support around areas of clinical nutrition to both families and other healthcare professionals. The neonatal dietetic role should continue following discharge, to support families with transition to home, weaning and optimising nutrition. Dietitians are key members of the MDT involved in supporting these vulnerable infants. Hazel Duncan, RD
Unlocking healthy infant development: the 'Thrive 5' factors

11th April 2024
A recent study from Washington University in St. Louis sheds light on the importance of what they term the 'Thrive 5' conditions for optimal infant development. These five crucial elements encompass environmental stimulation, nutrition, neighbourhood safety, positive caregiving and regular circadian rhythms and sleep.
Published in JAMA Pediatrics, the research underscores how these factors significantly influence brain development, cognitive abilities and social-emotional well-being in infants. Lead researchers Deanna Barch and Joan Luby, emphasise that providing these basic supports, even in challenging environments, positively impacts a child's development trajectory.
By studying 232 infants and their mothers, researchers observed that infants exposed to the Thrive 5 conditions displayed healthier developmental outcomes at age three, despite adverse circumstances. The study highlights the malleability of the brain to experience, and stresses the importance of prioritising these factors in US public health policy and paediatric care.
The researchers acknowledge the challenges parents face in providing these conditions, however, stressing the need for public policy interventions to ensure access to safe housing, adequate income and support systems for caregivers.
Prioritising the Thrive 5 factors may provide a solid foundation for healthy infant development, with far-reaching implications for lifelong well-being. It's certainly food for thought.
New research into the nutritional care of children and young people with acute lymphoblastic leukaemia
Lovell et al (2024) assessed the evolution of nutritional care in children and young people with acute lymphoblastic leukaemia (ALL). ALL is recognised to be the most common paediatric malignancy worldwide. While survival rates have improved, children and young people with ALL continue to face significant nutritional-related issues.
The study group looked at the advances in medical treatment for this group, the nutritional challenges faced, nutritional screening tools and the appropriateness of these, along with nutritional assessment, treatment and interventions. The group looked at energy requirement equations and the lack of an appropriate equation suitable specifically for this patient group. Nutritional goals were considered and they recommended looking at diet quality, not just calories alone. The study group identified there was a lack of dietetic input in survivorship groups. Short- and long-term impacts on bone health and the microbiome were also included.
From the information gathered, the group concluded that there is an increased number of overweight or obese children both at diagnosis and at completion of treatment. There are marked advances in medical treatment, which have led to improved survivor rates and the long-term nutritional goals for the children during treatment and beyond should be modified to reflect this and optimise overall health. Hazel Duncan, RD
Study Finds Waist-to-Height Ratio Superior to BMI in Detecting Fat Obesity in Children and Adolescents
A new study identifies waist circumference-to-height ratio as a more accurate measure of obesity in children and adolescents compared to BMI. Conducted by the University of Bristol, University of Exeter, and University of Eastern Finland, the research suggests this measure can better detect excess fat mass and differentiate it from muscle mass. Published in Pediatric Research, the study comes as childhood and adolescent obesity rates soar, affecting nearly 1 in 4 young people. Current methods like BMI often fail to distinguish between fat and muscle mass accurately, complicating obesity diagnosis and timely interventions. More here...
Childhood stress - risk of obesity and diabetes in adulthood
The largest brain study on childhood trauma, conducted by the University of Essex, led by Dr Megan Klabunde, reveals how it impacts development and alters crucial neural pathways. The research found disruptions in networks related to self-focus and problem-solving, suggesting that young people under 18 who have experienced abuse may struggle with emotions, empathy, and body awareness. Dr Klabunde's innovative use of AI analysed numerous brain scans to identify these patterns.
The study aims to inform the development of new treatments for mistreated children. This would potentially involve therapeutic techniques to rewire affected brain centres and reconstruct the child's self-perception.
Dr Klabunde hopes this study will be a springboard to find out more about how trauma affects developing minds. She said: "In addition to preventing avoidance of scary situations and addressing one's thoughts, trauma therapies in children should also address how trauma's impacts on one's body, sense of self, emotional/empathetic processing, and relationships. This is important to do so since untreated symptoms will likely contribute to other health and mental health problems throughout the lifespan."
Regular use of paracetamol during pregnancy may cause language delays in children

Regular use of acetaminophen, better known as paracetamol or Panadol in the UK and Tylenol in the US, can lead to language delays among children, according to a new study linked to the Illinois Kids Development Study.
Researchers from the University of Illinois Urbana-Champaign collected language data from a cohort of 532 two- and three-year-olds. During pregnancy, mothers were questioned every four to six weeks about their acetaminophen use and again 24 hours after giving birth. The researchers reported that acetaminophen in the second and third trimesters was linked to meaningful delays in early language development and each additional use of acetaminophen in the third trimester appeared to correlate with two fewer words in a two-year-old’s vocabulary. Whilst more studies are needed into this, previous studies have linked the use of acetaminophen during pregnancy to language delays and the risk of ADHD.
Preterm infants study: is human milk-based fortification more beneficial than bovine-based?
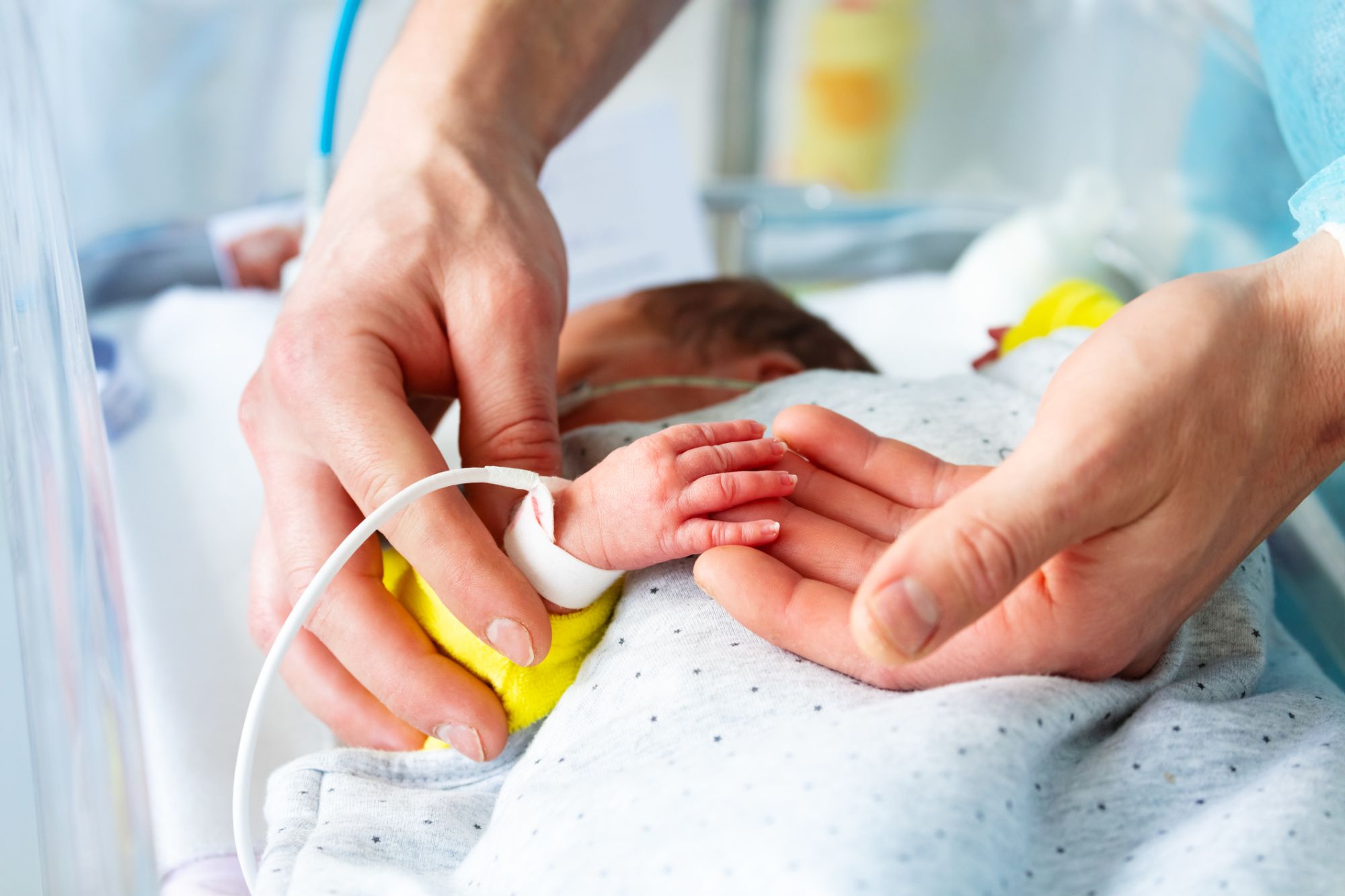
Extremely premature infants need to get nutrient enrichment over and above breast milk in order to thrive. This can be in the form of fortified cow's milk or donated breast milk. New research has investigated whether breast or bovine milk is best for lowering the risk of severe complications in these vulnerable babies.
A large Swedish study called N-Forte (the Nordic study on human milk fortification in extremely preterm infants) has just published its findings. Thomas Abrahamsson, Professor at Linköping University and Senior Physician at the neonatal department at the University Hospital led the current study. He says, "In Sweden, all extremely preterm infants receive breast milk from their mother or donated breast milk. Despite this, almost 1 in 10 children get a severe inflammation of the intestine called necrotising enterocolitis...At least 3 out of 10 children die and those who survive often have neurological problems afterwards,"
The N-Forte study looked into whether donated breast milk can reduce the risk of diseases in extremely preterm infants. The study included 228 extremely preterm infants, randomly divided into two equally-sized groups that received enrichment made from breast milk and cow's milk respectively. The researchers examined whether the two groups differed in the incidence of necrotising enterocolitis, sepsis and death. Hopwever, no difference was found between the groups. The full study can be found here...
To advertise on the NHD Paediatric Hub, please call 01342 824073 or e-mail [email protected].